Abstract
Purpose
Bronchial hemoptysis induced by intercostal pulmonary venous shunt (IPVS) is clinically rare. Pulmonary lesions on pleural surface may facilitate opening of vascular network. This retrospective study investigated safety and efficacy of embolization agents with small-particle embolization treating patients with massive hemoptysis due to IPVS.
Methods
Patients with massive hemoptysis (n = 207) underwent computed tomography angiography of bronchial artery. Depending on results, selective or superselective digital subtraction angiography and embolization were performed. Polyvinyl alcohol (300–500 μm), or microcoils combined with polyvinyl alcohol, was utilized according to IPVS volume. Vital signs of each patient were closely monitored.
Results
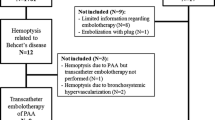
Of 207 patients with massive hemoptysis, 24 (11.6%) had IPVS syndrome. Patients with IPVS had concomitant bronchiectasis (54.2%), followed by tuberculosis (25.0%). Embolizations were performed in 39 culprit intercostal arteries; 37 (94.9%) of these were successfully embolized. Of the latter, 30 and 7 arteries were embolized, respectively, by polyvinyl alcohol alone or polyvinyl alcohol particles combined with microcoils. Embolization failed in one case because the agents could not enter the intercostal artery. If artery dissection occurred during procedure, microcoils were utilized to embolize the main artery. No skin necrosis, spinal artery embolization, or death occurred. Immediate clinical success was achieved in 22 patients (91.7%) after embolization. Two patients (8.3%) experienced recurrence of hemoptysis. Only four patients experienced mild hemoptysis during the 24-month follow-up with the efficiency of 75.0%.
Conclusions
Intercostal artery embolization with 300–500 μm alone or combined with microcoils is a safe and effective procedure in patients with IPVS-induced bronchial hemoptysis.


Similar content being viewed by others
References
Bhalla A, Kandasamy D, Veedu P, Mohan A, Gamanagatti S (2015) A retrospective analysis of 334 cases of hemoptysis treated by bronchial artery embolization. Oman Med J 30(2):119–128. https://doi.org/10.5001/omj.2015.26
Pei R, Zhou Y, Wang G, Wang H, Huang X, Yan X et al (2014) Outcomes of bronchial artery embolization for life-threatening hemoptysis secondary to tuberculosis. PLoS ONE 9(12):e115956. https://doi.org/10.1371/journal.pone.0115956
Chen J, Chen LA, Liang ZX, Li CS, Tian Q, Yang Z et al (2014) Immediate and long-term results of bronchial artery embolization for hemoptysis due to benign versus malignant pulmonary diseases. Am J Med Sci 348(3):204–209. https://doi.org/10.1097/MAJ.0000000000000226
Lu GD, Zu QQ, Liu XL, Wang B, Zhou CG, Xia JG et al (2016) Embolisation for life-threatening haemoptysis complicated by systemic artery-pulmonary circulation shunts. Int J Tuberc Lung Dis 20(2):276–281. https://doi.org/10.5588/ijtld.15.0078
Tintillier M, de Suray N, Alexis F, Mathy I, Rombaut E (2004) Systemic-to-pulmonary venous shunt in a haemodialysis patient. Nephrol Dial Transpl 19(10):2673. https://doi.org/10.1093/ndt/gfh351
Ittrich H, Klose H, Adam G (2015) Radiologic management of haemoptysis: diagnostic and interventional bronchial arterial embolisation. Rofo 187(4):248–259. https://doi.org/10.1055/s-0034-1385457
Fruchter O, Schneer S, Rusanov V, Belenky A, Kramer MR (2015) Bronchial artery embolization for massive hemoptysis: long-term follow-up. Asian Cardiovasc Thorac Ann 23(1):55–60. https://doi.org/10.1177/0218492314544310
Cornalba GP, Vella A, Barbosa F, Greco G, Michelozzi C, Sacrini A et al (2013) Bronchial and nonbronchial systemic artery embolization in managing haemoptysis: 31 years of experience. Radiol Med 118(7):1171–1183. https://doi.org/10.1007/s11547-012-0866-y
Larici AR, Franchi P, Occhipinti M, Contegiacomo A, del Ciello A, Calandriello L et al (2014) Diagnosis and management of hemoptysis. Diagn Interv Radiol 20(4):299–309. https://doi.org/10.5152/dir.2014.13426
Yoo DH, Yoon CJ, Kang SG, Burke CT, Lee JH, Lee CT (2011) Bronchial and nonbronchial systemic artery embolization in patients with major hemoptysis: safety and efficacy of N-butyl cyanoacrylate. AJR Am J Roentgenol 196(2):W199–W204. https://doi.org/10.2214/AJR.10.4763
Walker CM, Rosado-de-Christenson ML, Martinez-Jimenez S, Kunin JR, Wible BC (2015) Bronchial arteries: anatomy, function, hypertrophy, and anomalies. Radiographics 35(1):32–49. https://doi.org/10.1148/rg.351140089
Gu W, Sun LH, Fang SR, Ma JY, Zhang AP, Chen L (2007) Clinical analysis of the rare causes of hemoptysis: a report of 4 cases. Zhonghua Jie He He Hu Xi Za Zhi 30(5):343–346
Morais F, Almeida T, Campos P (2014) Arterio-arterial fistula between pulmonary and intercostal arteries–case report of “unilateral rib notching”. Rev Port Pneumol 20(3):167–171. https://doi.org/10.1016/j.rppneu.2013.08.004
Liu H, Zhang D, Zhang F, Yin J (2016) Immediate and long-term outcomes of endovascular treatment for massive hemoptysis. Int Angiol 35(5):469–476
Hwang HG, Lee HS, Choi JS, Seo KH, Kim YH, Na JO (2013) Risk factors influencing rebleeding after bronchial artery embolization on the management of hemoptysis associated with pulmonary tuberculosis. Tuberc Respir Dis (Seoul) 74(3):111–119. https://doi.org/10.4046/trd.2013.74.3.111
Baltacioglu F, Cimsit NC, Bostanci K, Yuksel M, Kodalli N (2010) Transarterial microcatheter glue embolization of the bronchial artery for life-threatening hemoptysis: technical and clinical results. Eur J Radiol 73(2):380–384. https://doi.org/10.1016/j.ejrad.2008.10.017
Navarro Esteva J, Perez Mendoza G, Pardo Moreno MD, Julia Serda G (2015) Skin necrosis as a complication of bronchial artery embolization. Rev Clin Esp 215(3):190–191. https://doi.org/10.1016/j.rce.2014.11.005
Pestana Knight EM, Novelli PM, Joshi SM (2011) Cerebral and systemic infarcts after bronchial artery embolization. Pediatr Neurol 45(5):324–327. https://doi.org/10.1016/j.pediatrneurol.2011.08.012
Ljudmila NO, Pesut D, Stevic R, Stojsic J (2007) Uncommon pulmonary infection with recurrent hemoptysis. Chin Med J (Engl) 120(24):2331–2333
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Yonghui LIANG declares that he has no conflict of interest. Yonghui LIANG declares that he has no conflict of interest. Wengjiang ZHAO declares that he has no conflict of interest. Jie TIAN declares that he has no conflict of interest. Fei CAI declares that he has no conflict of interest. Xiaolin ZHANG declares that he has no conflict of interest.
Ethical approval
This study was approved by the Medical Ethics Committee at the first Affiliated Hospital with China Three Gorges University and Ethics Committee/IRB (ethics no. 2017-001-04). Written informed consent was obtained from each included patient.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fu, Z., Liang, Y., Zhao, W. et al. Safety and efficacy of transcatheter embolization in patients with massive hemoptysis due to intercostal pulmonary venous shunts. Radiol med 124, 588–594 (2019). https://doi.org/10.1007/s11547-019-01020-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-019-01020-0